Rhiannon Osborne
60% of voters regard the National Health Service (NHS) as the most important factor influencing their vote[i]. In the past few weeks, the NHS has repeatedly come to the forefront of the UK’s General Election debates, with the price of drugs becoming an increasingly high-profile topic.
This issue, however, goes far beyond any political party. It is part of a much wider debate on the power of pharmaceutical companies, the correct pricing of drugs, and the effect that free marketing pricing has on our access to medicines. So – how do trade, drugs and the UK General Election fit into the bigger picture?
What’s the ‘deal’ with drug pricing?
World Health Organisation believes 2 billion people do not have access to essential medicines[ii]. This is partly due to the high price of medicines globally, both for individuals facing out-of-pocket payments and for governments purchasing medicines for their health services.
The current profit model of the pharmaceutical industry is such that once a company develops a drug, they may be granted a patent, which lasts for 20 years, allowing them to be the only producer and seller of this drug during that period. Patents are a part of intellectual property law which is set at a national level. However, patents are also governed by international treaties and bi-lateral trade agreements. With this monopoly, a drug company has the ability to charge high prices without facing competition.
This opportunity is rarely wasted – in the US in 2017, one gram of Gilead’s Hepatitis C treatment, Sofosbuvir, cost 67 times more than a gram of gold[iii]. In 2013, the pharmaceutical industry generated more profit than any other industry globally[iv]. However, once a drug reaches the market, it barely costs more than the raw ingredients to manufacture. So, why the need for huge profits?
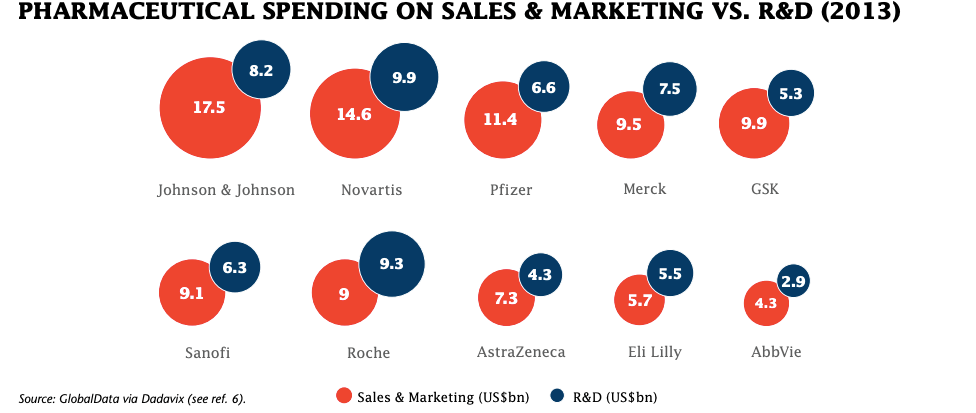
Pharmaceutical companies claim that high prices are necessary for the drug developer to re-coup the cost of researching and developing the drug. This claim has been extensively debunked due to, amongst other reasons, the high levels of public investment into drug research and the lack of reinvestment of profits into further research[v]. In fact, nearly all drug companies spend more on marketing and share buybacks (to increase their own stock prices) than they do on researching new drugs[vi].
Once the patent runs out, generic drug manufacturers can enter the market, which can reduce drug prices by up to 80%. This incentivises drug manufacturers to extend their monopolies, for example by applying for multiple patents on the same drug and preventing competitor companies from using their clinical trial data. Additionally, pharmaceutical companies often advocate for more restrictive patent law at the national and international level. This can prevent countries from using public health safeguard measures to improve access to medicines.
UK drug pricing – how could it change?
Drug prices in the UK are usually controlled by government regulation, whereas in many other countries, pharmaceutical companies set the prices. In the UK, the National Institute for Health and Care Excellence (NICE) assesses the benefits of a particular drug and decides the acceptable cost. The NHS then negotiates with a pharmaceutical company, usually achieving prices that are lower than the market price due to its significant size and bargaining power[vii]. NHS drug prices are capped by a voluntary pricing scheme, which prevents unpredictable increases in the prices of branded drugs[viii]. Mechanisms such as this constrain how much profit can be made on pharmaceutical sales in the UK.
The US has frequently voiced its desire to improve the ability of US firms to profit from the UK pharmaceutical market[ix]. Trump has previously criticised countries who attempt to control the price of drugs, arguing that they are avoiding paying their share of development costs[x]. The Trump administration argues that other countries must agree to pay more for American drugs so that the US can cut the cost of medication domestically, which is currently the highest in the world[xi].

American and British pharmaceutical companies are both pushing to change the way the UK agrees on the price of drugs[xiii],[xiv]. The US pharmaceutical industry has argued against the centralised government value assessments by NICE and urged government trade representatives to include changes to the assessment process, valuation and pricing[xv],[xvi]. Given the formidable power of the US pharmaceutical lobby (individual companies within the pharmaceuticals and health products sector reportedly spent $194.3 million on lobbying in 2018[xvii]), it is likely that US trade negotiators will try to meet some of their demands. The NHS voluntary pricing cap, in particular, is one of many price controls that seem unlikely to survive a free trade deal with the US[xviii].
As well as direct changes in drug pricing, the US is likely to push for stronger intellectual property rights. Demands in this area may include longer patent terms, making it easier to obtain patents, and increased clinical trial data exclusivity, which could delay NHS access to cheaper generic medicines[xix].
If these demands are met, they are almost guaranteed to affect drug pricing in the UK. The NHS confederation, which represents most hospital trusts in England, warned that demands made by the US could result in a large medicines bill and deny the NHS the opportunity to utilise cheaper alternatives to the expensive branded drugs[xx].
What have the major political parties said?
The Conservatives have consistently said that the NHS is “not on the table” in trade deals post Brexit[xxi]. However, the words “drug” and “prices” don’t have to be on the table for drug pricing to be affected.
UK officials sometimes use other terms, including ‘valuing innovation’ to avoid discussing drug pricing directly[xxii]. Furthermore, a former high-level trade negotiator for Trump said that he didn’t understand what the Prime Minister meant when he said that the NHS wasn’t “on the table”[xxiii]. Labour have repeatedly stated that the Conservatives would “sell our NHS to the United States and big pharma”, and have pledged to exclude the NHS, medicines and public services from any trade deals, and make this binding in law[xxiv].
Drug pricing has already been discussed between UK and US trade officials. A recent documentary revealed that British trade officials have held undeclared, unofficial meetings with American pharmaceutical corporations, and US trade negotiators, to discuss drug pricing. A freedom of information request into the contents of the meetings was initially met with a nearly entirely blacked out document[xxv], but the unredacted documents have since been leaked. According to analysis by Global Justice Now[xxvi], the talks show US officials making a further threat to NHS in terms of medicine pricing policy, with special concern about the price of cancer medicines.
Green Party MP Caroline Lucas said that the Conservative party can “no longer claim that NHS is not for sale”[xxvii] and Jeremy Corbyn stated that “these documents confirm that the US is demanding that the NHS is on the table in trade talks”[xxviii]. Although these documents are discussions, and by no means a finalised trade agreement, they do suggest that the US is trying to use various tactics to get the NHS to pay more money to US pharmaceutical companies for the drugs they sell.

Even with the best intentions, any future government may struggle to avoid concessions in a US-UK free trade agreement. The US has a formidable reputation for including issues related to pharmaceuticals in their foreign policy and has secured significant pro-pharma wins in their recent trade agreements with Canada, Mexico and South Korea[xxx]. The UK is especially likely to be forced into concessions given the size and significance of the NHS, and will likely be the weaker negotiating party post-Brexit, especially in the event of no-deal[xxxi].
Could the pharmaceutical industry be different?
The current model of drug development has multiple flaws other than the price of essential drugs and the power of pharmaceutical companies. For example, the monopoly-based system funnels research into drugs that are the most profitable, but not those that would make the most difference to public health.
There is a dearth of research into diseases that mostly affect the Global South, which represent a huge proportion of the global disease burden, because of the lack of a profitable market. Similarly, despite the urgent public health need for new antibiotics, research and development into new antibiotics has stifled in the last decades due to several ‘market failures’.

This problem is global, but not nationally insurmountable. An example of how a national government could restructure the system is Labour’s ‘Medicines for the Many’ policy[xxxii]. The policy proposes economic and regulatory incentives that could reconfigure the industry agenda to one that serves patients, not just shareholders. Public ownership of pharmaceuticals is the most frequently discussed proposal, but this is not as radical as it sounds. Several governments, including those of Brazil and Thailand, have successfully manufactured essential medicines for many years through nationalised production mechanisms.
Immediate actions that any government could take to improve access to medicines in the UK include:
- Using well established public health safeguard measures to overcome patent monopolies
- Placing affordability conditions on public money going into drug development and
- Requiring drug manufacturers to be transparent about the actual cost of research.
Changes in the assessment and regulation of pharmaceuticals have also been proposed by the Green Party[xxxiii].The Labour policy also argues that since the public sector already spends a lot of money buying and researching drugs, why not use this money to create the right amount of profit in the right places?
A key part of this idea is an exploration of a ‘de-linkage’ approach to health innovation in the UK. ‘De-linkage’ refers to an innovation model that rewards the costs and risks of research, but in a way that does not depend on financial returns coming from high product prices and patent protection. Public money and financial rewards could be concentrated in areas where the public health need is greatest, rewarding true innovation, not just market sales. These proposals have significant support from civil society, patients and industry professionals.

Policies that support a public-health focused research agenda and help to control drug prices globally would enable a transition to a system that places human lives over excessive profit. In this scenario, we could probably worry less about our post-Brexit trade deals.
What next?
There are many aspects of the cost of healthcare that this article has not considered, from the effect of Brexit on EU medicines to the future of privatisation within the NHS. What is clear, however, is that the profit made on the sales of drugs strains healthcare systems and gives the pharmaceutical industry an excessive amount of influence over international politics. Regardless of whoever wins the election, this will not be the last time the public is worried about the cost of healthcare. It begs the question – is something as essential as health suited to free-market economics, or do we need some better ideas?
[i] https://www.mirror.co.uk/news/politics/boost-jeremy-corbyn-nhs-overtakes-20921849
[ii] https://www.who.int/publications/10-year-review/chapter-medicines.pdf?ua=1
[iii] https://msf.lu/en/news/focus/hepatitis-c-the-cost-of-eradicating-the-disease
[iv] https://www.bbc.co.uk/news/business-28212223
[v] https://www.msfaccess.org/lives-edge-time-align-medical-research-and-development-peoples-health-needs
[vi] https://www.msf.org/6-things-big-pharma-doesn%E2%80%99t-want-you-know-access-medicines
[vii] https://www.bbc.com/news/health-50295231
[viii] https://www.fiercepharma.com/pharma/pharma-caps-u-k-s-branded-drug-spend-growth-at-2-exchange-for-faster-access
[ix] https://ustr.gov/sites/default/files/Summary_of_U.S.-UK_Negotiating_Objectives.pdf
[x] https://pharmaphorum.com/news/corbyn-accuses-tories-of-planning-deal-to-hike-drug-prices-with-trump-as-election-looms/
[xi] https://www.theguardian.com/politics/2019/nov/01/nhs-drugs-bill-could-soar-if-johnson-signs-trump-trade-deal-report
[xii] https://www.ntd.com/trump-administration-announces-plan-allowing-people-to-buy-lower-cost-prescription-drugs-from-canada_363955.html
[xiii] https://www.scotsman.com/news/politics/brexit-uk-government-criticised-for-secret-trade-meetings-with-us-drugs-firms-1-5034602
[xiv] https://www.abpi.org.uk/media/7515/analysis-would-medicines-for-the-many-lead-to-many-medicines.pdf
[xv] http://phrma-docs.phrma.org/sites/default/files/pdf/fact-sheet-nice-restrictiveness.pdf
[xvi] https://www.scotsman.com/news/politics/brexit-uk-government-criticised-for-secret-trade-meetings-with-us-drugs-firms-1-5034602
[xvii]https://www.opensecrets.org/federal-lobbying/industries/summary?cycle=2019&id=H04
[xviii] https://pharmaphorum.com/news/corbyn-accuses-tories-of-planning-deal-to-hike-drug-prices-with-trump-as-election-looms/
[xix] https://www.nhsconfed.org/-/media/Confederation/Files/Publications/Documents/REPORT_The-NHS-and-future-free-trade-agreements23Sept19.pdf
[xx] https://www.theguardian.com/politics/2019/nov/01/nhs-drugs-bill-could-soar-if-johnson-signs-trump-trade-deal-report;
[xxi] https://www.telegraph.co.uk/politics/2019/10/29/make-no-mistake-beloved-nhs-will-never-table-trade-deal-usa/
[xxii] https://www.independent.co.uk/news/uk/politics/nhs-us-trade-deal-trump-boris-johnson-healthcare-drug-prices-liz-truss-a9175261.html
[xxiii] https://pharmaphorum.com/views-analysis-market-access/secret-us-uk-talks-on-drug-pricing-revealed/
[xxiv] https://www.theguardian.com/society/2019/nov/16/nhs-us-pharma-donald-trump-selloff
[xxvii] https://www.bbc.co.uk/news/uk-politics-50572454;
[xxviii] https://www.mirror.co.uk/news/politics/breaking-jeremy-corbyn-reveals-451-20970436?fbclid=IwAR1UUQI0mOyU2xDXpX88JLnBxNkGdhus1jOYTUNcAosWn-_djYEEGpBO_cM
[xxix] https://www.yahoo.com/now/labour-claims-nhs-at-risk-of-privatisation-under-us-uk-trade-deal-103623766.html?guccounter=1&guce_referrer=aHR0cHM6Ly93d3cuZ29vZ2xlLmNvLnVrLw&guce_referrer_sig=AQAAADE65a657GWigRjPAsEmguX0aMA1aiilwJVYuy6KkFTcsahzbiWFSOewlSF0QKjUANwwhGv1rI_79iHB2ZzXELkJpf-mbkve6YbEHAhdlkbqDLilEe8RHlz4UEkdhHX7YkGeAEv5SvhtqtCJexLLdTm6vlxi0S4GgocGKrgGt5DU
[xxx] https://www.newstatesman.com/politics/uk/2019/06/uk-has-much-fear-us-trade-agreement
[xxxi] https://www.independent.co.uk/news/uk/politics/nhs-us-trade-deal-trump-boris-johnson-healthcare-drug-prices-liz-truss-a9175261.html
[xxxii] http://labour.org.uk/wp-content/uploads/2019/09/Medicines-For-The-Many.pdf

One thought on “Pharmaceutical Power and the General Election”